2-year-old experiencing 50 seizures per day finds relief through surgery
[anvplayer video=”5148698″ station=”998122″]
The scar on two-year-old Hudson Kroll’s hairline is barely noticeable as he plays in his family’s Eagan home. In mid-September, he underwent brain surgery to remove a mass caused by tuberous sclerosis complex (TSC).
“Looking back, I feel like everything went so smoothly and he’s a little miracle,” said Melissa Kroll, Hudson’s mother.
In January, Hudson fell and hit his head on their coffee table. The swelling and bogginess of the injury caused his mother, who is a nurse, to bring him to the hospital.
A CT scan of his brain revealed Hudson had a mass. After additional tests at Children’s Minnesota, he was diagnosed with TSC. The genetic condition causes the growth of tubers, which are noncancerous tumors that can cause seizures.
“After his first seizure, we got seizure meds right away and kept trying medication after medication,” said Kroll, who said Hudson started to decline developmentally. “Before seizures he would say ‘Mama’ and ‘Dada’ and he would use utensils to eat his food and after the seizures started we slowly noticed he stopped being able to use a fork and spoon and he stopped saying the few words he did know.”
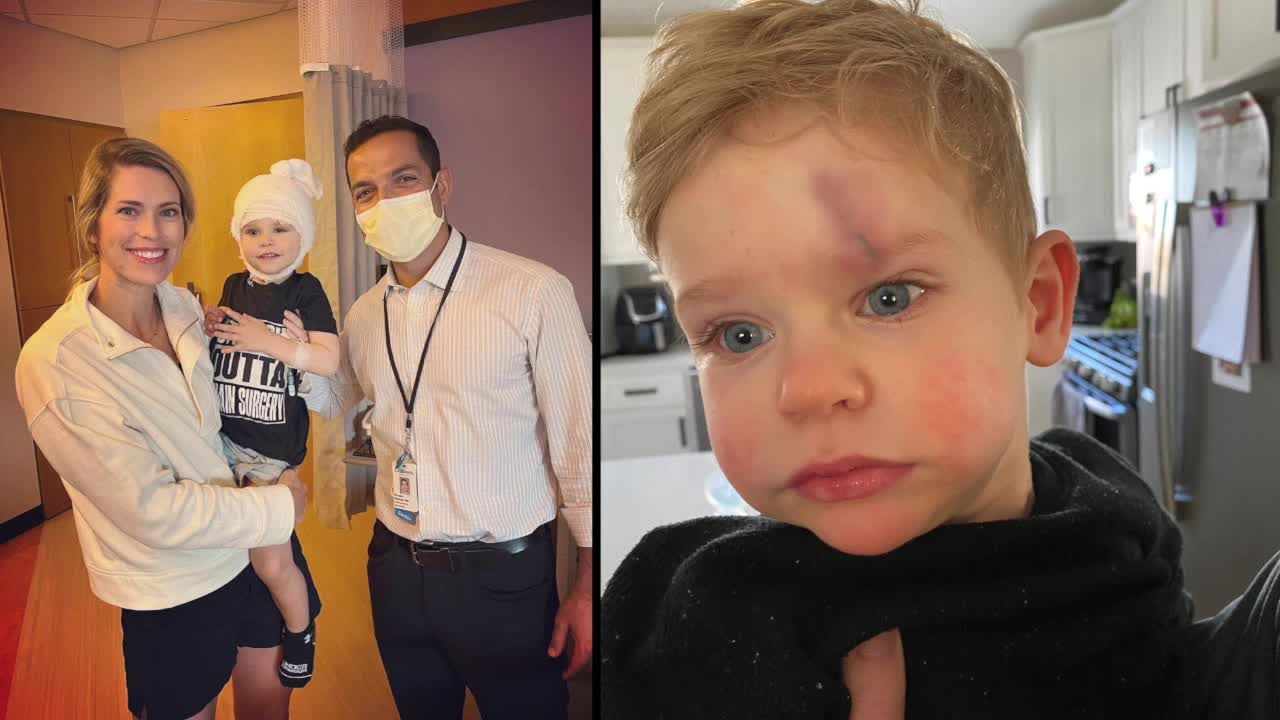
(Photos courtesy of the Kroll family)
They started re-evaluating their treatment plan as Hudson’s seizures continued.
“I think probably by the third or fourth medication we were trying different things and nothing was really working,” said Jeff Kroll, Hudson’s father.
Those changes were tracked by a team at Children’s Minnesota. The Level 4 Epilepsy Center includes Children’s Minnesota experts and Minnesota Epilepsy Group employees.
Dr. Meysam Kebriaei, the director of neurosurgery at Children’s Minnesota, walked the Krolls through the possibility of brain surgery.
“At that point he was having about 50 seizures a day so very devastating to both him and his family,” said Dr. Kebriaei, who gave Hudson a 70% to 80% chance of being seizure-free after surgery.
While they were initially hesitant to pursue the operation, the Krolls moved forward with the open resection craniotomy in mid-September. They hoped it would bring Hudson some relief.
According to experts with the Minnesota Epilepsy Group, their team only performs one open resection craniotomy in TSC patients approximately every year or two. They treat about 160 patients, both adults and children, with TSC each year.
“When you’re a parent and you hear they’re going to be taking something out, especially in the brain, you just worry he’s not going to be the same kid when he comes out of it,” said Jeff Kroll. “It’s just miraculous that even when you take something out how he can change for the positive.”
The tuber was located in the front left part of Hudson’s brain, which Dr. Kebriaei described as an area “with minimal risk”.
“We registered exactly where my incision was going to be, where his tuber was before we even made our incision,” he said. “We removed part of the bone and we were able to remove just the right amount of bone — not too much, not too little — using that navigation system.”
Dr. Kebriaei explained how cutting edge technology also allowed them to identify the abnormal tissue and remove it while protecting healthy brain tissue. Once they removed the tuber, an MRI was brought into the operating room for another scan.
“A door opens, we all leave, we cover the patient and then the MRI machine comes in,” he said, pointing to rails on the ceiling that guide the machine in the operating room. “To make sure we removed all the tuber and that there’s not a blood clot or other complications there.”
When no issues were identified, doctors returned to the room.
“We all go back into the room then we close and put the bone back on with absorbable plate and screws,” Dr. Kebriaei explained.
His team removed the entire tuber. Hudson hasn’t had a seizure since the surgery.
“The chances of this coming back is pretty close to zero,” he said. “He has a very good chance of never having seizures again.”
Hudson was awake within an hour of the procedure. He started speaking the next day and was running the halls of the hospital on the second day following surgery, according to his parents.
“The day after surgery he said ‘Mama’ for the first time since before his seizures started, I think that just gave us all chills,” said Melissa Kroll.
As his doctors track his progress, Hudson’s parents are grateful physicians were able to intervene so early. His doctors were able to identify his TSC because he hit his head exactly where the mass was.
“He didn’t his head hard enough to have this large mass here so when they first initially did the scan it was really questioning what that was and that’s what prompted the MRI,” said Jeff Kroll.
The diagnosis allowed them to recognize Hudson’s seizures.
“They were very subtle, where he just looks like he’s checking out or is unfocused,” said Kroll. “If we hadn’t known that he had this genetic disorder, we wouldn’t have known they were seizures at all and who knows how long they would’ve gone on for.”
Hudson now has speech, occupational and physical therapy three days a week to catch up on what he lost.
“It’s like he’s coming out of this fog that he was in prior to surgery,” said Melissa Kroll.
Jeff added, “I feel like this was his pathway back to who he really is as a kid.”
For more information about treatment options for epilepsy, click here.